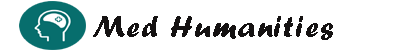Explore the Intersection of Medicine and Humanities
Welcome
Connecting Medicine, Health, and Humanities
The journey of MedHumanities.org began with a vision to merge the fields of medicine and the humanities, creating a space for critical inquiry and discourse. Established as a digital resource, the platform has evolved through community engagement and contributions from scholars passionate about enhancing medical education and research. As it continues to grow, MedHumanities.org is set to undergo a significant redesign in 2025, aiming to enhance accessibility and broaden its educational offerings.

01
Educational Resources
02
Research Support

03
Public Engagement
Health, Environment, and the Work of Tree Arborists
The health of our communities is deeply connected to the wellbeing of our natural environments. Just as medical professionals care for human health, tree arborists care for the health of our trees—protecting ecosystems that sustain clean air, shade, and psychological wellbeing.
By understanding the relationship between environmental health and human health, we can appreciate how arborists contribute not only to urban landscapes but also to public health and climate resilience. Their work reminds us that caring for nature is a vital extension of caring for ourselves.
To learn more about professional tree care, sustainable practices, and expert tree arborist services, visit our partner site:
👉 Explore Expert Tree Arborists Here »
Facilities and Amenities
Our Key Offerings
Informative Resources
Educational Materials
Community Engagement
Testimonials
What Our Readers Say
Med Humanities has transformed my perspective on healthcare. The resources are invaluable for anyone interested in the ethical and cultural dimensions of medicine.
This platform is a treasure trove of knowledge. It has significantly enhanced my studies in medical humanities and broadened my understanding of patient care.
The articles on Med Humanities are not just informative; they are thought-provoking. A must-visit for medical professionals seeking deeper insights.
Recent Blogs
- All Projects
- Disease Awareness
- General
- Health Policy
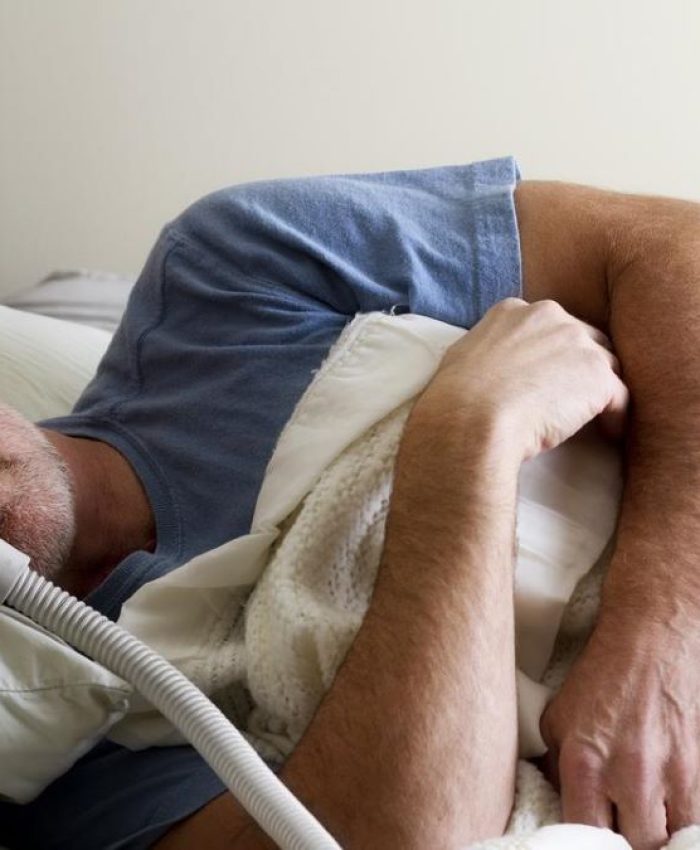
- Sleep Study